The Most Promising 3D Bioprinting Projects

Bioprinting is a method that makes it possible to manufacture cellular structures from bioinks loaded with stem cells: layer by layer, the biomaterial is deposited to design skin, tissue or even an organ. Imagine a 3D printed heart, ear, lung or kidney, custom-designed with the patient’s own cells. What a breakthrough for the medical sector! It is still a bit early to count on bio-printed organs that are viable and durable over time, which is the challenge for our researchers. But progress is making great strides and in the long run, bioprinting could help us to face the lack of organ donors or simply to better understand certain pathologies. Here, we have selected some of the main bioprinting projects in the world, whether they are 3D printed tissues, organs or body parts.
A 3D Printed Mini Human Heart Which Beats
A Boston University research team has used 3D printing technology to develop a miniature replica of a human heart. The device was created using a combination of human stem cell-derived heart cells and microscale 3D printed acrylic parts. It is a “precision-enabled miniaturized unidirectional cardiac microfluidic pump,” also known as miniPUMP (miniaturized Precision-enabled Unidirectional Microfluidic Pump).The amazing feature of the miniPUMP is that it can beat on its own, just like a human heart, thanks to its living tissue.
Researchers want to use this replica of the heart chamber to study how the heart works in the human body. The device could, for example, be used to better understand how the heart grows in an embryo, how heart tissue is affected by disease, or how effective new drugs are in treating such diseases. A true revolution that could avoid the need for human testing in the future.

Photo: Left: A large-scale replica of the 3D-printed scaffold that supports heart tissue. (Photo credit: Christos Michas). Right: A side view image of the miniPOMPA taken in the lab. (Photo credit: Jackie Ricciardi).
A 3D-Printed Solution for Kidney Failure
We discover another prime example of bioprinting in relation to kidneys. Countless people around the world suffer from its failure, but just as badly, there aren’t exactly many options for treatment. That’s why U.S.-based Trestle Biotherapeutics has been working to develop 3D-printed tissue that can be implanted into patients suffering from end-stage renal disease. Specifically, this is completely functional kidney tissue that is designed to replace and also supplement previously lost kidney function. According to Trestle Biotherapeutics, this new therapy works by integrating stem cell biology in combination with 3D bioprinting. The goal of the Trestle team is not only to free patients from dialysis treatment and give them more time before transplantation, but also to use this bioprinted kidney tissue as a functional replacement organ in the future.
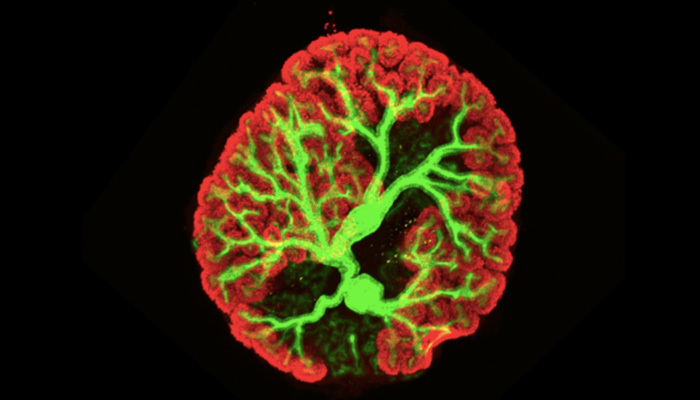
Photo credit: Trestle Biotherapeutics
3D Printing of a Cornea Could Help Eye Disease
Every year, more than 1.5 million people suffer from corneal problems that can lead to blindness. To address this, a research group in Hyderabad, India, has successfully completed the development of the first 3D bioprinted cornea. The tissue itself has been manufactured from a bioink obtained from human corneal tissue and without the addition of any other artificial or synthetic elements. Those in charge of the initiative claim that, for every human cornea donated, three new corneas can be 3D printed. These advances in the field of ophthalmology will help treat diseases such as corneal scarring and keratoconus. The project has been tested in rabbits and, although there is still some time before it can be used in humans, the results have been successful and very promising.
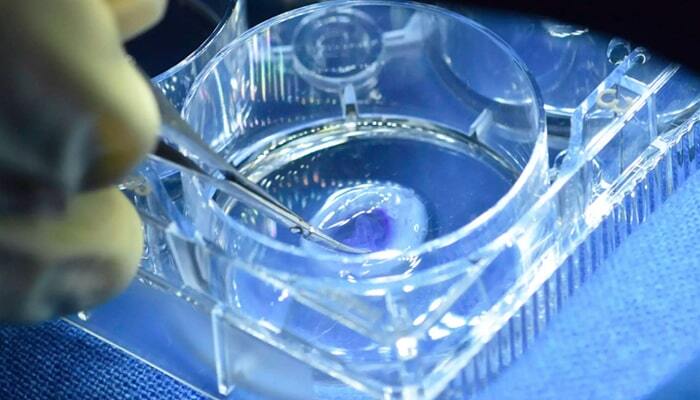
Photo credit: IANS Photo
A 3D Bioprinted Ovary for Insight into Women’s Healthcare
Women’s health is a field of medicine often considered to be under researched; there are many conditions which are currently not well understood. However, 3D bioprinting of parts of the reproductive system could help scientists to better understand cell behavior and, in turn, various diseases. In 2022, a group of scientists based at Tongi Hospital in China developed a 3D printed artificial ovary using cells from mice and Gelatin methacryloyl (GelMA), a common hydrogel used in bioengineering. They found that this hydrogel was a viable choice for 3D bioprinting. The results suggested that it was not suitable for primary ovarian cells (meaning ovarian cells harvested directly from tissue). However, it was suitable for the growth in vitro of ovarian follicles, (that is, a group of cells containing an immature egg cell and other cells). According to the researchers, their results could be clinically applied ‘ in the treatment of female endocrine and reproductive condition[s]’.
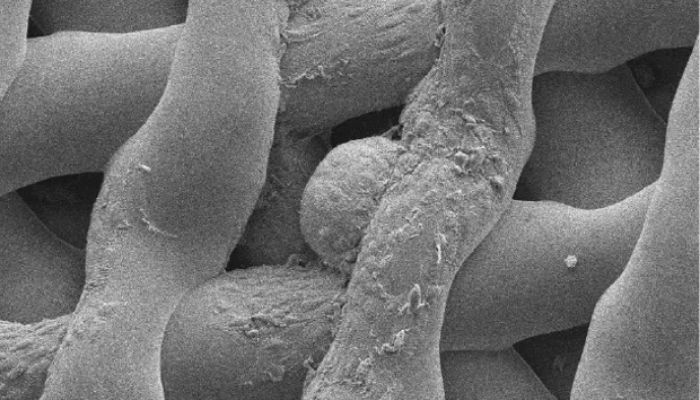
In a similar project at Northwestern University, scientists grew a mouse egg cell in a bioprosthetic ovary scaffold. (Photo credit: Northwestern University)
Bioprinting a Mini Liver in Only 90 Days
Researchers at the University of São Paulo in Brazil have succeeded in creating miniature versions of a human liver from blood cells. The process took only 90 days, from the collection of the patient’s blood to the production of the tissue. These liver organoids, developed using 3D bioprinting technologies, integrate the functionalities of the 3D printed organ in question. These include the production of vital proteins, the storage of vitamins and the secretion of bile. To create the liver tissue, the team used the Inkredible bioprinter, marketed by the manufacturer CELLINK, one of the most recognized in the industry.
A Bioprinted Ear Project Helps a Young Girl Regain Hearing
A young woman from the USA suffering from microtia was successfully transplanted with a 3D-printed ear. The condition is a congenital anomaly that impedes the development of the outer ear. The implant was made by the company 3DBio Therapeutics from collagen hydrogel and cartilage cells from the patient. As little as half a gram is sufficient for cartilage harvesting from the ear. The cells responsible for cartilage formation are cultivated in a patented nutrient mixture and multiply as a result. These are then mixed with a bio-ink. Within 10 minutes, an ear can be printed for patients. After the printing process, the ear is shipped in a protective case to the surgeon, who then performs the transplantation.
Unlike the traditional treatment method, in which a prosthesis is made from rib cartilage, this treatment is less costly. Professor Anthony Atala, Director of the Wake Forest Institute for Regenerative Medicine emphasizes the importance of this project: “This is a major breakthrough for the field of regenerative medicine. 3D printing aims to offer a number of advantages over handmade artificial tissue, including scaling, higher design accuracy and lower cost.”

Photo credit: 3DBio Therapeutics
A Bioprinted Pancreas to Help Fight Diabetes
The pancreas plays an important role in the body as it is responsible for insulin production. As a result, when it malfunctions, it can have serious consequences, namely causing diabetes. Given that the disease affects more than 463 million people worldwide, the drive to find more permanent and effective solutions to curing diabetes is becoming more important and 3D printing especially could play a role. For example, the Polish company Polbioionica. A spin out from a multidisciplinary team of scientists from the Foundation for Research and Development of Science who were the first to use bioprinting to make a bionic pancreas with a full vascular system back in March 2019, the company is dedicated to creating this fully functional organs out of proprietary bioinks and pancreatic islets, as well as the patient’s own stem cells. They hope the tailor-made solution will not only provide a solution to the ever worsening organ shortage worldwide, but could prevent the development of complications in people who suffer from diabetes, all while reducing healthcare expenses.
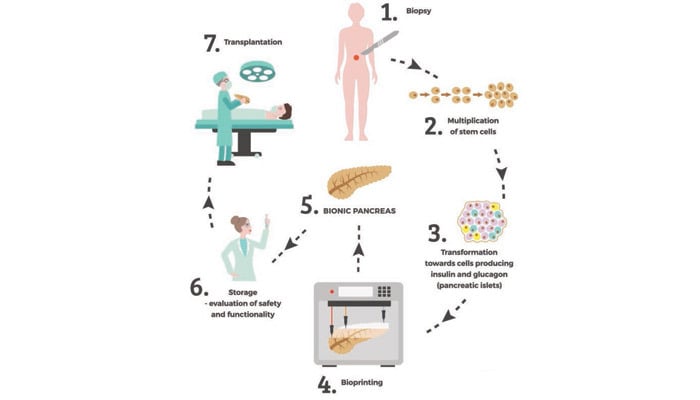
Photo Credits: Fundacja Badań i Rozwoju Nauki
Poietis and its 3D Bio-printed Skin Project
Poietis is a French company specialized in 3D bioprinting solutions. It designs and markets a range of 3D bioprinters called Next Generation Bioprinting. The company is particularly well known for its research work on skin. Poietis presents the Poieskin, a full thickness human skin model entirely produced by 3D bioprinting. In detail, this skin is made up of a dermal compartment, one of the three layers of the skin between the epidermis and the hypodermis, composed of fibroblasts, cells of the dermis, embedded in type 1 collagen and covered by an epidermis arranged in superimposed layers that give rise to a 3D pattern. This 3D bioprinted skin could be used by anyone who has suffered severe burns, cancer or other accidents. According to Poietis, the high precision and resolution of their 3D bioprinter allows for the fabrication of controlled 3D cellular structures and reproducible skin tissue models. Recently, the French manufacturer was able to conduct their first clinical trial with their 3D bioprinter. It has also installed the Next Generation Bioprinting platform in a hospital to manufacture implantable biological tissues.
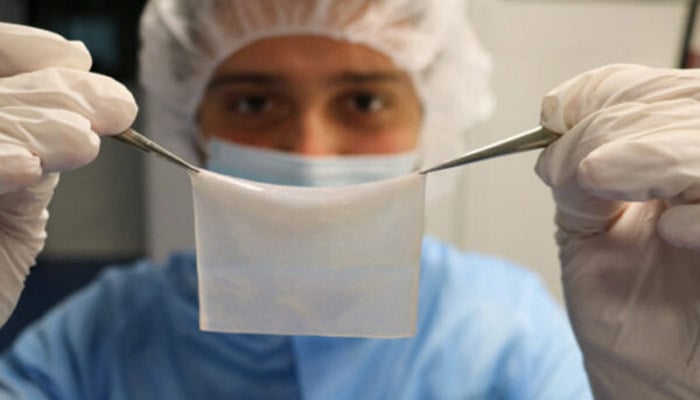
Photo credit: Poeitis
The First 3D Printed Nose Reconstruction
There are a number of reasons why a patient could require prosthetics, especially if they are suffering from diseases which may need surgery. And though of course treating illness is most important, it can be difficult for the patient to suddenly change their appearance. Luckily, bioprinting may also be able to solve this issue. In a case from the Toulouse University Cancer Institute and CERHUM, a patient who had lost a large part of her nose as well as the front part of her palate during treatment for nasal cavity cancer, was able to essentially grow her own nose, allowing for a complete reconstruction, done by Dr. Agnes Dupret-Bories and Dr. Benjamin Vairel. The process to do this had a number of steps, starting with a 3D printed biomaterial that was implanted under the skin on the patient’s forearm for vascularization, or the process of growing blood vessels into a tissue. After two months, the colonization of the medical device was complete and it was transplanted to the nasal area and successfully revascularized, giving the patient a fully working nose, made out of her own cells.
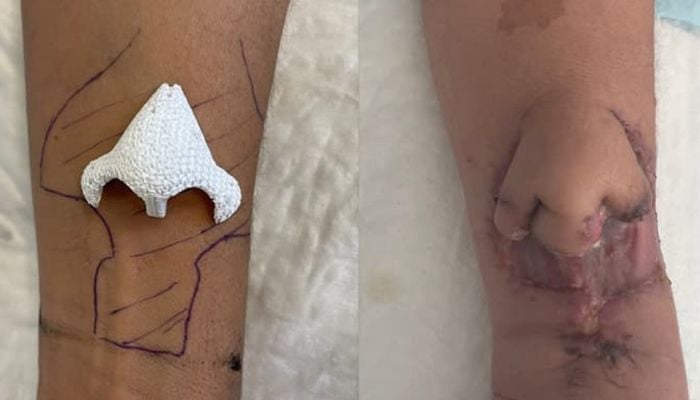
Photo Credits: CERHUM/Toulouse University Hospital
If you prefer videos, you can find more exciting applications of 3D bioprinting in our clip below.
What do you think of these 3D bioprinting projects to make bioprinted organs? Let us know in a comment below or on our LinkedIn, Facebook, and Twitter pages! Don’t forget to sign up for our free weekly Newsletter here, the latest 3D printing news straight to your inbox! You can also find all our videos on our YouTube channel.









i like plastic skin